Bladder Stones: When to Seek Treatment and Why Timing Matters
Struggling with urinary problems? Find out whether bladder stones could be the reason and what to do next.
13 March 20268m


A mild burning sensation, frequent trips to the bathroom or the feeling that your bladder never fully empties can be easy to dismiss. Most people assume it is a passing infection or simple irritation. Yet for some, these familiar symptoms are the earliest signs of a condition that has troubled humans for thousands of years.
Bladder stones are not a modern health issue. Archaeologists have found them in Egyptian mummies dating back more than 5,000 years, as documented in research published by the National Library of Medicine, evidence of just how persistent and serious this problem can be. Despite advances in medicine, bladder stones still affect people today, often silently, until discomfort turns into disruption.
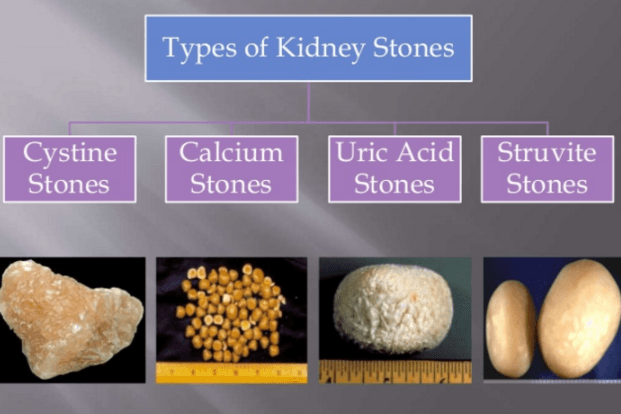
In the UK, bladder stones are less common than kidney stones, but they remain a significant concern, particularly among men over 50, according to the NHS. Bladder stones are hard mineral masses formed in the bladder, most commonly composed of uric acid (often in men with concentrated urine) or calcium (oxalate/phosphate).
Other types include struvite stones (linked to chronic infections) and rare cystine stones(genetic).
Conditions such as prostate enlargement can interfere with normal bladder emptying, allowing stones to develop and grow over time. Ignoring bladder stones does more than prolong discomfort. In severe or long-standing cases, chronic bladder irritation and obstruction may even increase the risk of bladder cancer, as highlighted in clinical literature indexed by the National Institutes of Health.
For many patients, access to prompt care remains a challenge. Lengthy NHS waiting times can mean living with worsening urinary symptoms for weeks or even months, during which stones may continue to enlarge. Discomfort, urgency, and obstruction often intensify while patients wait, increasing the likelihood that treatment becomes more complex. What might have been manageable early on can, over time, develop into a serious risk to bladder health and overall quality of life.
Hidden Urinary Problems That Lead to Bladder Stones
Bladder stones usually develop as a result of underlying urinary problems rather than forming on their own. Identifying these root causes is essential, as treating the stone alone without correcting the underlying issue significantly increases the risk of recurrence. Without proper evaluation and targeted management, many patients experience repeated bladder stone formation even after successful treatment.
- Incomplete Bladder Emptying: This allows urine to remain in the bladder, promoting stone formation; in men, this is often linked to prostate enlargement, while in women, it may result from bladder or pelvic floor dysfunction.
- Blocked or Slowed Urine Flow: Any narrowing or obstruction in the urinary tract can slow urine flow, allowing minerals to settle and clump together over time instead of being flushed out naturally.
- Repeated Urinary Tract Infections (UTIs): Ongoing infections can change the chemical balance of urine, making it easier for crystals to form and grow into stones, especially when infections are not fully resolved.
- Long-Term Catheter Use: Prolonged catheter placement can allow minerals to collect on its surface, increasing the risk of bladder stone formation over time.
- Previous Bladder or Prostate Surgery: Surgical changes to the bladder or prostate can disrupt normal urine flow or bladder emptying, increasing the risk of stone formation.
- Low Fluid Intake: Not drinking enough fluids can lead to concentrated urine, which increases the risk of mineral buildup and stone formation.
However, as stones grow, they can irritate the bladder lining, cause pain, and interfere with normal urine flow. Bladder stones often develop silently; understanding how they form and recognising early warning signs is essential for timely diagnosis and effective treatment.
When Small Symptoms Signal a Bigger Bladder Problem
The signs and symptoms of bladder stones often depend on their size and movement within the bladder. Early symptoms may be mild and easy to overlook, which is why many people delay seeking medical advice. Symptoms that persist for more than two weeks or gradually worsen should never be ignored, even if they seem minor at first.
Common symptoms of bladder stones include:
- Pain or burning during urination
- Frequent urge to urinate, especially at night
- Difficulty starting or stopping urine flow, or a weak stream
- Lower abdominal or pelvic pain
- Cloudy or dark-coloured urine
- Blood in the urine
Early symptoms can often go unnoticed, and with extended NHS waiting times, delays in assessment may allow stones to grow larger, causing increased bladder irritation or complications. Prompt assessment can prevent small stones from developing into more complex cases that require invasive treatment. Since symptom severity often relates to stone size, understanding how the size of a bladder stone affects symptoms and treatment decisions is particularly important.
The Bigger the Stone, the Bigger the Risk
Bladder stones vary significantly in size, and stone size plays a major role in determining risk, symptoms, and treatment complexity. As stones grow, they are more likely to cause obstruction, pain, and infections, often with a sudden worsening of symptoms.
- Small-sized stones: These may be as small as grains of sand and often cause mild, intermittent or no symptoms at all. Because discomfort is minimal, patients may delay seeking medical attention. Small stones can sometimes be managed with minimally invasive procedures.
- Medium-sized stones: As stones increase in size, symptoms become more noticeable. Patients may experience pain while urinating, difficulty emptying the bladder or repeated urinary tract infections. Treatment at this stage is usually more involved and may require specialised endoscopic procedures.
- Large stones: Larger stones are associated with a higher risk of urine blockage, severe pain, and recurrent infections. They rarely pass on their own and typically require surgical intervention, making treatment more complex and recovery longer.
In healthcare systems like the NHS, where waiting times for urology assessments and procedures can be extended, delays in evaluation may allow stones to grow larger, potentially making treatment more complex. Since self-assessment is unreliable, timely medical evaluation and accurate diagnosis are essential to determine stone size and plan the safest, most effective treatment.
Why Bladder Stones Should Never Be Self-Diagnosed
Bladder stones may seem straightforward, but accurate diagnosis is crucial to prevent complications, plan effective treatment, and reduce the risk of recurrence. Doctors need to confirm the presence of stones, assess their size, number, and location, and identify any underlying urinary problems.
- Clinical Evaluation and Symptom Review: Diagnosis starts when symptoms like painful urination, frequent urge, difficulty emptying the bladder, or blood in the urine prompt medical attention. Doctors review symptoms, medical history, and risk factors to determine which investigations are needed.
- Urine Tests: Urine analysis can detect blood, crystals or infection, providing early clues about stone presence. While these tests cannot confirm stones alone, they guide further investigation.
- Imaging Tests: Imaging is the most reliable way to visualise stones and assess their size and location. These findings directly influence both the urgency and type of treatment recommended. Ultrasound is a common first-line, non-invasive method. X-rays or CT scans offer precise information on the number, size and position of stones, which is critical for planning treatment.
- Endoscopic Examination (Cystoscopy): For complex or recurrent cases, a cystoscope- a thin camera inserted through the urethra- allows doctors to directly examine stones and the bladder lining. This is particularly important for larger stones or those that keep coming back.
Accurate and timely diagnosis ensures that doctors can choose the safest, most effective treatment, prevent complications such as obstruction or infection, and determine stone size, number, and exact location. All critical factors in deciding the appropriate treatment approach. Delays in diagnosis can allow stones to increase in size, making treatment more complex and recovery longer.
Why One Treatment Doesn’t Fit All the Bladders
Treatment for bladder stones is tailored to the individual, taking into account stone size, number, location, severity of symptoms, and overall health. Personalised treatment planning improves outcomes and reduces unnecessary procedures. After diagnosis, patients often want to understand all available options and how each may affect outcomes, recovery, and long-term bladder health.
- Endoscopic (Minimally Invasive) Stone Removal: For small bladder stones, endoscopic procedures are often the preferred approach. A thin instrument is inserted through the urethra to visualise and remove the stone. In some cases, stones are first broken into smaller fragments before extraction. This approach is less invasive, has a shorter recovery time, and allows patients to resume daily activities quickly.
- Percutaneous or Surgical Stone Removal: Larger stones or stones that cannot be safely removed endoscopically may require surgical intervention. This involves directly accessing the bladder to remove the stone completely. Surgical removal ensures all stones are eliminated, reducing the risk of complications such as urinary obstruction, recurrent infections, or bladder damage.
- Effective treatment also focuses on correcting the factors that caused the stones, such as an enlarged prostate, urinary obstruction, or recurrent infections. Managing these issues reduces the likelihood of stone recurrence and supports long-term bladder health.
What Recovery Really Looks Like After Bladder Stone Treatment
Recovery after bladder stone treatment depends on how the stone is removed and whether any underlying urinary problems are addressed. Patients who receive early treatment generally experience faster recovery and fewer post-procedure complications. In the UK, the most common procedures are endoscopic (minimally invasive) removal, where stones are broken down and extracted through the urethra, and open surgery for larger or more complex stones.
- Hospital Stay: Patients undergoing endoscopic procedures such as transurethral or percutaneous cystolitholapaxy usually stay in the hospital for a few days. Those undergoing open bladder surgery (cystostomy) may require a longer hospital stay before they are well enough to return home.
- Follow-Up Care: Recovery does not end at discharge. Follow-up appointments are essential, and imaging tests like X-rays or CT scans may be used to confirm that all stone fragments have been completely removed. Skipping follow-up care increases the risk of recurrence and persistent symptoms. Even small leftover fragments can serve as a base for new stones, so this step is critical.
- Long-Term Recovery and Bladder Health: With timely diagnosis and appropriate treatment, patients generally experience smoother recovery, fewer complications, and a lower risk of recurrence. Early treatment also limits prolonged bladder irritation and inflammation, which can otherwise delay healing and increase long-term risks. Managing contributing factors such as prostate enlargement, bladder outlet obstruction, or long-term catheter use further supports recovery and helps maintain long-term bladder health.
Navigating Bladder Stone Care with Confidence
While bladder stones are often treatable with modern medical techniques, outcomes depend heavily on how early the condition is diagnosed and managed. When care is delayed, stones can grow larger, symptoms can worsen, and lead to complications. Timely access to specialist care can significantly improve comfort, recovery and long-term bladder health. In the UK, access to specialist urology care can sometimes be affected by waiting times, referral delays, or limited availability of advanced procedures, even when symptoms are disruptive. For many patients, this gap between diagnosis and treatment can significantly impact comfort, recovery, and overall quality of life.

For patients seeking prompt and coordinated care, The Medical Travel Company (TMTC) helps navigate patients to accredited hospitals, experienced urologists, and structured treatment plans. This is particularly important for patients whose symptoms are worsening or who cannot afford prolonged delays in care, such as lengthy NHS waiting lists. Beyond arranging procedures, TMTC supports patients with aftercare, follow-up appointments, and ongoing guidance, providing continuity and peace of mind throughout their bladder stone treatment journey. A coordinated approach ensures treatment decisions are timely, appropriate, and focused on long-term bladder health rather than short-term relief.
Sources:
- NCBI- https://www.ncbi.nlm.nih.gov/books/NBK441944/
- NHS- https://www.nhs.uk/conditions/bladder-stones/treatment/
- NCBI- https://pmc.ncbi.nlm.nih.gov/articles/PMC2778769/